Featured Articles

Safeguarding Against Diabetes-Related Amputations
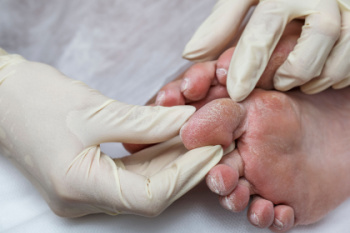
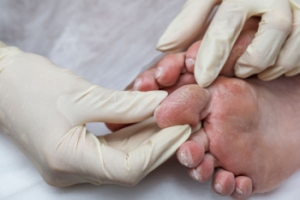
Diabetes-related amputations pose a grave threat to individuals grappling with this chronic condition, but preventive measures can help to reduce this risk. Consistent blood sugar management is essential, and maintaining target levels through a balanced diet, regular exercise, and medication adherence can significantly reduce the likelihood of complications. Routine foot care is equally as vital, as inspecting feet daily for cuts, blisters, or infections and promptly treating any abnormalities can prevent minor issues from escalating. Wearing well-fitted shoes and socks can safeguard against pressure sores and friction-related injuries. Avoiding barefoot walking minimizes exposure to potential hazards. Regular visits to a podiatrist for foot examinations and professional care are imperative for early detection and intervention. Additionally, prioritizing cardiovascular health by managing blood pressure and cholesterol levels aids in preserving overall vascular function, reducing the risk of peripheral artery disease and subsequent amputations. By implementing these preventive strategies, individuals with diabetes can safeguard their feet and minimize the threat of amputations. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can present you with additional information about protecting your feet from amputation.
Diabetic Limb Salvage
Diabetic limb salvage can be an effective way in preventing the need for limb amputation. If you have a foot ulcer and diabetes, consult with one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Diabetic Limb Salvage?
Diabetic limb salvage is the attempt of saving a limb, such as the foot, that has an infected ulcer, from amputation. Podiatrists also try to make sure that there is enough function in the foot after the salvage that it is still usable. Those with diabetes experience poor blood circulation, which prevents proper healing of an ulcer. If the ulcer is left uncheck, it could become infected, which could result in the need for amputation.
Diabetes is the number one cause of non-traumatic amputations in the United States. Amputation has been found to lead to higher mortality rates. This translates into higher healthcare costs, and a reduced quality of life and mobility for amputees. Podiatrists have attempted to increase the prevalence of limb salvage in an attempt to solve these issues.
Diagnosis and Treatment
Limb salvage teams have grown in recent years that utilize a number of different treatments to save the infected limb. This includes podiatrists that specialize in wound care, rehabilitation, orthotics, and surgery. Through a combination of these methods, limb salvage has been found to be an effective treatment for infected limbs, and as an alternative to amputation. Podiatrists will first evaluate the potential for limb salvage and determine if the limb can be saved or must be amputated.
If you have any questions, please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Diabetic Limb Salvage
Limb salvage is a procedure that involves saving a lower extremity from amputation. In podiatry, limb amputation often occurs as a result of diabetes. The fundamental goal of limb salvage is to restore and maintain stability and movement of the affected lower extremity.
The procedure typically involves removing the diseased tissue and a small portion of the surrounding healthy tissue, as well as the removal of any affected bone if necessary. If bone is removed it is then replaced with prostheses, or synthetic metal rods or plates, or grafts from either the patient’s body or a donor. Limb salvage is typically the preferred choice of procedure over amputation, as the procedure preserves both the patient’s appearance and allows for the greatest possible degree of function in the affected limb.
Upon diagnosis and determining that limb salvage is the appropriate treatment, the podiatrist may enlist the help of a physical and/or occupational therapist to prepare the patient for surgery by introducing various muscle-strengthening, walking, and range of motion exercises. Such exercises may be continued as rehabilitation post-procedure.
Definition and Causes of an Achilles Tendon Rupture
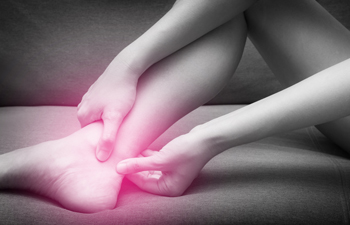
Achilles tendon rupture, a distressing injury affecting the tendon at the back of the ankle, can be debilitating and necessitate prompt attention. This critical tendon connects the calf muscles to the heel bone, facilitating movement like walking, running, and jumping. When subjected to excessive force or strain beyond its capacity, the Achilles tendon can tear partially or completely, resulting in a rupture. These types of injuries are frequently observed during activities involving sudden bursts of acceleration, abrupt changes in direction, or inadequate warm-up routines. Athletes, particularly those engaging in sports demanding rapid movements or high-impact activities, are at increased risk. Additionally, factors such as age weakened tendons due to degeneration, improper footwear, and inadequate conditioning contribute to susceptibility. Recognizing the signs and symptoms, including a sudden sharp pain in the heel, swelling, and difficulty walking or pointing toes downward, is vital for early diagnosis. If you have endured an Achilles tendon rupture, it is strongly suggested that you consult a podiatrist who can offer you effective treatment methods.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact one of our podiatrists of Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Achilles Tendon Injuries
The Achilles tendon is the largest tendon in the body; it is a tough band of fibrous tissue that stretches from the bones of the heel to the calf muscles. This tendon is what allows us to stand on our toes while running, walking, or jumping, it is common for this tendon to become injured. In severe cases, the Achilles tendon may become partially torn or completely ruptured. However, this tendon is susceptible to injury because of its limited blood supply and the high level of tension it endures.
The people who are more likely to suffer from Achilles tendon injuries are athletes who partake in activities that require them to speed up, slow down, or pivot. Consequently, athletes who engage in running, gymnastics, dance, football, baseball, basketball, or tennis are more likely to suffer from Achilles tendon injuries. Additionally, there are other factors that may make you more prone to this injury. People who wear high heels, have flat feet, tight leg muscles or tendons, or take medicines called glucocorticoids are more likely to have Achilles tendon injuries.
A common symptom of an Achilles tendon injury is pain above the heel that is felt when you stand on your toes. However, if the tendon is ruptured, the pain will be severe, and the area may become swollen and stiff. Other symptoms may be reduced strength in the lower ankle or leg area, and reduced range of motion in the ankle. When the Achilles tendon tears, there is usually a popping sound that occurs along with it. People who have acute tears or ruptures may find walking and standing to be difficult.
If you suspect you have injured your Achilles tendon, you should see your podiatrist to have a physical examination. Your podiatrist will likely conduct a series of tests to diagnose your injury including a “calf-squeeze” test. Calf squeeze tests are performed by first squeezing the calf muscle on the healthy leg. This will pull on the tendon and consequently cause the foot to move. Afterward, the same test will be performed on the injured leg. If the tendon is torn, the foot won’t move because the calf muscle won’t be connected to the foot.
Who Is Vulnerable to Developing Gout?
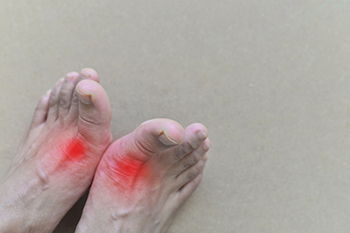
Gout, often characterized by sudden and intense pain, swelling, and redness in the joints, primarily affects individuals who exhibit certain predisposing factors. Men over the age of 40 are particularly susceptible, as are postmenopausal women due to hormonal changes. Additionally, those with a family history of gout are at an increased risk, suggesting a genetic component to the condition. Lifestyle choices can also play a significant role. Excessive alcohol consumption, particularly beer, and a diet rich in purine-containing foods such as red meat, seafood, and organ meats can elevate the risk. Additionally, obesity and conditions like high blood pressure, diabetes, and kidney disease are associated with a higher likelihood of developing gout. Taking certain medications, such as diuretics, can contribute to elevated uric acid levels, increasing the likelihood of gout flare-ups. If you have had one or more gout attacks, it is strongly suggested that you are under the care of a podiatrist who can help you to manage this condition.
Gout is a painful condition that can be treated. If you are seeking treatment, contact one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Everything You Need to Know About Gout
Gout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint.
The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
This form of arthritis, being particularly painful, is the leftover uric acid crystallizing in the blood stream. The crystallized uric acid then travels to the space between joints where they rub, causing friction when the patient moves. Symptoms include: pain, redness, swelling, and inflammation. Additional side effects may include fatigue and fever, although reports of these effects are very rare. Some patients have reported that pain may intensify when the temperature drops, such as when you sleep.
Most cases of gout are easily diagnosed by a podiatrist’s assessment of the various symptoms. Defined tests can also be performed. A blood test to detect elevated levels of uric acid is often used as well as an x-ray to diagnose visible and chronic gout.
Treatment for gout simply means eliminating symptoms. Non-steroid anti-inflammatory drugs or NSAIDs (Colchicine and other corticosteroid drugs, etc.) will quell the redness, the swelling, and the inflammation. However, managing your diet, lifestyle changes, and using preventative drugs are all helpful toward fully combating the most severe cases.
Those that lead an inactive lifestyle are at a higher risk for gout. Any amount of exercise decreases the probability of repeat encounters with the condition. Reducing your consumption of red meat, sea food, and fructose-sweetened drinks also reduces the likelihood of chronic gout as well.
Ingesting Vitamin C, coffee, and particular dairy products can help with maintaining a healthy lifestyle. There are new drugs out on the market that inhibit the body’s production of uric acid-producing enzymes. However, reducing or eliminating your overall levels of uric acid is the best remedy to ensuring you lead a gout-free life.
Non-Diabetic Foot Ulcers
Non-diabetic foot ulcers are open sores or wounds that occur on the feet of individuals who do not have diabetes. While less common than diabetic foot ulcers, they still pose significant health risks. These ulcers can develop due to things like poor circulation, trauma, pressure, or infections. People at risk include those with peripheral artery disease, venous insufficiency, neuropathy, or autoimmune conditions. Additionally, lifestyle factors like smoking, obesity, and a sedentary lifestyle can increase the risk. Non-diabetic foot ulcers often manifest as painful lesions, typically on the bottom of the foot or toes. They require prompt medical attention to prevent complications such as infection or tissue damage. Treatment may involve wound care, infection management, pressure relief, and addressing underlying conditions contributing to ulcer formation. If you have sores on your feet that won't heal, it is strongly suggested that you schedule an appointment with a podiatrist as quickly as possible for a comprehensive treatment plan.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Causes of Stress Fractures in the Foot
 Stress fractures in the foot are tiny cracks in the bone that happen when your feet are overworked. Unlike regular fractures that occur from a single, severe impact, stress fractures result from repetitive force over time, like running long distances or jumping repeatedly. Athletes and people who dramatically increase physical activity without proper training are more likely to develop stress fractures. After muscles are pushed to a certain point, they become fatigued and place extra stress to the bones, leading to these small cracks. Poor footwear, uneven surfaces, and weak bones from conditions like osteoporosis can increase the risk of developing stress fractures. Pain with stress fractures in the foot often worsens over time and may be experienced as a dull achy feeling. If you have sustained a stress fracture in the foot, it is suggested you make an appointment with a podiatrist promptly for treatment.
Stress fractures in the foot are tiny cracks in the bone that happen when your feet are overworked. Unlike regular fractures that occur from a single, severe impact, stress fractures result from repetitive force over time, like running long distances or jumping repeatedly. Athletes and people who dramatically increase physical activity without proper training are more likely to develop stress fractures. After muscles are pushed to a certain point, they become fatigued and place extra stress to the bones, leading to these small cracks. Poor footwear, uneven surfaces, and weak bones from conditions like osteoporosis can increase the risk of developing stress fractures. Pain with stress fractures in the foot often worsens over time and may be experienced as a dull achy feeling. If you have sustained a stress fracture in the foot, it is suggested you make an appointment with a podiatrist promptly for treatment.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.