Featured Articles

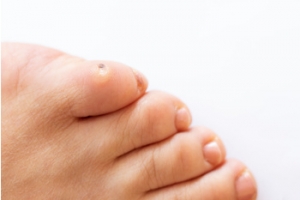
Treatment for Foot Corns
 Corns are thickened skin areas that form to protect the skin against friction and pressure, and often occur on the feet. A podiatrist, or foot doctor, may recommend changing to footwear that fits better and doesn't squeeze or rub against the foot. Additionally, they might recommend padding or cushions to protect the corn and reduce pressure when walking. In more persistent cases, a podiatrist may carefully trim the thickened skin using a scalpel, a procedure that should never be attempted at home because of the risk of infection. Custom foot orthotics may also be suggested to correct any foot abnormalities that contribute to corn formation. Along with proper foot hygiene, these treatments can effectively manage and prevent the discomfort associated with corns. If you are struggling with corns on the feet, it is suggested that you consult a podiatrist for help.
Corns are thickened skin areas that form to protect the skin against friction and pressure, and often occur on the feet. A podiatrist, or foot doctor, may recommend changing to footwear that fits better and doesn't squeeze or rub against the foot. Additionally, they might recommend padding or cushions to protect the corn and reduce pressure when walking. In more persistent cases, a podiatrist may carefully trim the thickened skin using a scalpel, a procedure that should never be attempted at home because of the risk of infection. Custom foot orthotics may also be suggested to correct any foot abnormalities that contribute to corn formation. Along with proper foot hygiene, these treatments can effectively manage and prevent the discomfort associated with corns. If you are struggling with corns on the feet, it is suggested that you consult a podiatrist for help.
Corns can make walking very painful and should be treated immediately. If you have questions regarding your feet and ankles, contact one of our podiatrists of Romeo Foot & Ankle Clinic. Our doctors will treat your foot and ankle needs.
Corns: What Are They? And How Do You Get Rid of Them?
Corns are thickened areas on the skin that can become painful. They are caused by excessive pressure and friction on the skin. Corns press into the deeper layers of the skin and are usually round in shape.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as:
- Wearing properly fitting shoes that have been measured by a professional
- Wearing shoes that are not sharply pointed or have high heels
- Wearing only shoes that offer support
Treating Corns
Although most corns slowly disappear when the friction or pressure stops, this isn’t always the case. Consult with your podiatrist to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Understanding Corns and Calluses
Corns and Calluses are both hardened layers of thickened skin that develop because of friction. Both ailments are typically found on the feet and may be unsightly. Although they have similarities, corns and calluses are different from each other.
Some causes of corns and calluses may be wearing ill-fitting shoes and not wearing socks. If you wear tight shoes, your feet will constantly be forced to rub against the shoes, causing friction. If you fail to wear socks, you are also causing your feet to endure excess friction.
There are some signs that may help you determine whether you have one of these two conditions. The first symptom is a thick, rough area of skin. Another common symptom is a hardened, raised bump on the foot. You may also experience tenderness or pain under the skin in addition to flaky, dry, or waxy skin.
There are also risk factors that may make someone more prone to developing corns and calluses. If you are already dealing with bunions or hammertoe, you may be more vulnerable to having corns and calluses as well. Other risk factors are foot deformities such as bone spurs, which can cause constant rubbing inside the shoe.
Corns tend to be smaller than calluses and they usually have a hard center surrounded by inflamed skin. They also tend to develop on the parts of the body that don’t bear as much weight such as the tops and sides of toes. Corns may also be painful for those who have them. On the other hand, calluses are rarely painful. These tend to develop on the bottom of the feet and may vary in size and shape.
Fortunately, most people only need treatment for corns and calluses if they are experiencing discomfort. At home treatments for corns and calluses should be avoided, because they will likely lead to infection. If you have either of these ailments it is advised that you consult with your podiatrist to determine the best treatment option for you.
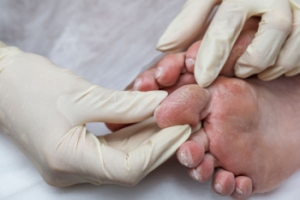
Origins of Blisters on the Feet

Blisters on the feet can be an unwelcome nuisance, often causing discomfort and hindering mobility. These fluid-filled sacs typically form in response to friction or repetitive rubbing against the skin. When excessive pressure or irritation occurs, the outer layer of the skin separates from the underlying tissue, creating a protective bubble filled with fluid. Common culprits behind blister formation include wearing ill-fitting shoes, prolonged periods of walking or running, and friction caused by sweaty or damp conditions. Additionally, certain activities, such as hiking or wearing new shoes without proper breaking in, can increase the likelihood of developing blisters. Individuals with foot deformities or abnormalities may also be more prone to blister formation due to uneven pressure distribution. If you have a blister on your foot that has become infected, it is suggested that you consult a podiatrist who can safely treat it and provide effective prevention techniques for future knowledge.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact one of our podiatrists of Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blisters
Blisters are small pockets of fluid that occur on the top layers of the skin for several reasons. Friction, burns, and diseases are all known causes of blisters. Smaller blisters are known as vesicles, while larger blisters are referred to as bulla. The fluid inside the bubble can be blood, pus, or serum; which is a clear liquid that protects the skin. In most cases, blisters are not a major health issue, but they can be an indicator of a more serious condition.
Causes of blisters vary. Blisters are commonly caused by wearing poorly fitted shoes that rub against the foot. However, there are many other causes besides from friction; including burns, sunburn, insect bites, frostbite, poison ivy/oak, chemical exposure, impetigo, eczema, viral infections, and more.
Most blisters heal by themselves and do not require immediate medical care. If you have a blister, do not pop it since this may cause infection; it is advised to put a bandage over the blister to protect it. If the blister is large, causes pain, or if you have a fever, it is recommended that you see a doctor who can provide proper care. Blisters are easy to diagnose, and if considered prudent by the doctor, can easily be drained of fluid with a sterile needle as well.
To prevent blisters on the feet, wear shoes that fit properly and don’t cause rubbing. Socks can help prevent friction and it is recommended that you wear them if you are wearing shoes. Hand blisters can be avoided by wearing gloves during activities that cause friction against the hand. If you have a blister that pops, do not remove the dead skin, wash the area, apply antibiotic ointment, and cover with a bandage. It is okay in most cases to not seek immediate medical care for a blister if it was just caused by friction. However, if the blister causes pain or does not go away, it is suggested that you see a doctor for a diagnosis.
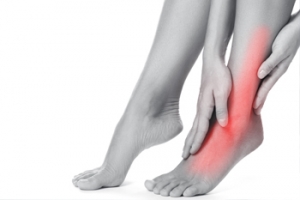
Causes of Foot Pain at Night
Foot pain at night can disrupt your sleep and affect your overall quality of life, leaving you restless and uncomfortable. Understanding the underlying causes is crucial for finding relief and improving your well-being. One common culprit is plantar fasciitis, characterized by inflammation of the tissue connecting the heel to the toes. This condition often leads to sharp, stabbing pain in the heel or arch, particularly when getting out of bed in the morning or after long periods of rest. Another potential cause is neuropathy, a nerve disorder that can result from conditions like diabetes or vitamin deficiencies. Neuropathic pain may present as burning, tingling, or shooting sensations in the feet, worsening at night when lying down. Additionally, arthritis, stress fractures, and overuse injuries can contribute to nocturnal foot pain. Identifying the specific cause through proper diagnosis by a healthcare professional is essential for implementing targeted treatment strategies and finding relief from nighttime foot discomfort. If you have foot pain at night, it is suggested that you make an appointment with a podiatrist for care.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
Our feet are arguably the most important parts of our bodies because they are responsible for getting us from place to place. However, we often don’t think about our feet until they begin to hurt. If you have pain in your feet, you need to first determine where on the foot you are experiencing it to get to the root of the problem. The most common areas to feel pain on the foot are the heel and the ankle.
Heel pain is most commonly attributed to a condition called plantar fasciitis. Plantar fasciitis occurs when the plantar fascia, which is the band of tough tissue connecting the heel bone to the toes becomes inflamed. Plantar fasciitis pain is usually worse in the morning, and it tends to go away throughout the day. If you have plantar fasciitis, you should rest your foot and do heel and foot muscles stretches. Wearing shoes with proper arch support and a cushioned sole has also been proven to be beneficial.
Some common symptoms of foot pain are redness, swelling, and stiffness. Foot pain can be dull or sharp depending on its underlying cause. Toe pain can also occur, and it is usually caused by gout, bunions, hammertoes, ingrown toenails, sprains, fractures, and corns.
If you have severe pain in your feet, you should immediately seek assistance from your podiatrist for treatment. Depending on the cause of your pain, your podiatrist may give you a variety of treatment options.
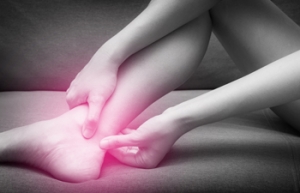
Safeguarding Against Diabetes-Related Amputations
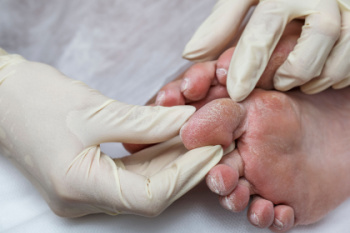
Diabetes-related amputations pose a grave threat to individuals grappling with this chronic condition, but preventive measures can help to reduce this risk. Consistent blood sugar management is essential, and maintaining target levels through a balanced diet, regular exercise, and medication adherence can significantly reduce the likelihood of complications. Routine foot care is equally as vital, as inspecting feet daily for cuts, blisters, or infections and promptly treating any abnormalities can prevent minor issues from escalating. Wearing well-fitted shoes and socks can safeguard against pressure sores and friction-related injuries. Avoiding barefoot walking minimizes exposure to potential hazards. Regular visits to a podiatrist for foot examinations and professional care are imperative for early detection and intervention. Additionally, prioritizing cardiovascular health by managing blood pressure and cholesterol levels aids in preserving overall vascular function, reducing the risk of peripheral artery disease and subsequent amputations. By implementing these preventive strategies, individuals with diabetes can safeguard their feet and minimize the threat of amputations. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can present you with additional information about protecting your feet from amputation.
Diabetic Limb Salvage
Diabetic limb salvage can be an effective way in preventing the need for limb amputation. If you have a foot ulcer and diabetes, consult with one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Diabetic Limb Salvage?
Diabetic limb salvage is the attempt of saving a limb, such as the foot, that has an infected ulcer, from amputation. Podiatrists also try to make sure that there is enough function in the foot after the salvage that it is still usable. Those with diabetes experience poor blood circulation, which prevents proper healing of an ulcer. If the ulcer is left uncheck, it could become infected, which could result in the need for amputation.
Diabetes is the number one cause of non-traumatic amputations in the United States. Amputation has been found to lead to higher mortality rates. This translates into higher healthcare costs, and a reduced quality of life and mobility for amputees. Podiatrists have attempted to increase the prevalence of limb salvage in an attempt to solve these issues.
Diagnosis and Treatment
Limb salvage teams have grown in recent years that utilize a number of different treatments to save the infected limb. This includes podiatrists that specialize in wound care, rehabilitation, orthotics, and surgery. Through a combination of these methods, limb salvage has been found to be an effective treatment for infected limbs, and as an alternative to amputation. Podiatrists will first evaluate the potential for limb salvage and determine if the limb can be saved or must be amputated.
If you have any questions, please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Diabetic Limb Salvage
Limb salvage is a procedure that involves saving a lower extremity from amputation. In podiatry, limb amputation often occurs as a result of diabetes. The fundamental goal of limb salvage is to restore and maintain stability and movement of the affected lower extremity.
The procedure typically involves removing the diseased tissue and a small portion of the surrounding healthy tissue, as well as the removal of any affected bone if necessary. If bone is removed it is then replaced with prostheses, or synthetic metal rods or plates, or grafts from either the patient’s body or a donor. Limb salvage is typically the preferred choice of procedure over amputation, as the procedure preserves both the patient’s appearance and allows for the greatest possible degree of function in the affected limb.
Upon diagnosis and determining that limb salvage is the appropriate treatment, the podiatrist may enlist the help of a physical and/or occupational therapist to prepare the patient for surgery by introducing various muscle-strengthening, walking, and range of motion exercises. Such exercises may be continued as rehabilitation post-procedure.
Definition and Causes of an Achilles Tendon Rupture
Achilles tendon rupture, a distressing injury affecting the tendon at the back of the ankle, can be debilitating and necessitate prompt attention. This critical tendon connects the calf muscles to the heel bone, facilitating movement like walking, running, and jumping. When subjected to excessive force or strain beyond its capacity, the Achilles tendon can tear partially or completely, resulting in a rupture. These types of injuries are frequently observed during activities involving sudden bursts of acceleration, abrupt changes in direction, or inadequate warm-up routines. Athletes, particularly those engaging in sports demanding rapid movements or high-impact activities, are at increased risk. Additionally, factors such as age weakened tendons due to degeneration, improper footwear, and inadequate conditioning contribute to susceptibility. Recognizing the signs and symptoms, including a sudden sharp pain in the heel, swelling, and difficulty walking or pointing toes downward, is vital for early diagnosis. If you have endured an Achilles tendon rupture, it is strongly suggested that you consult a podiatrist who can offer you effective treatment methods.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact one of our podiatrists of Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.