Featured Articles

Symptoms and Causes of Plantar Fasciitis

Foot pain can significantly disrupt daily activities and diminish quality of life, and plantar fasciitis is one of the main culprits. The plantar fascia is a thick band of tissue that stretches from the heel to the toes, supporting the foot’s arch and helping with movement. When this tissue becomes inflamed, it results in plantar fasciitis. This causes sharp heel pain that is especially noticeable with the first steps in the morning or after long periods of inactivity. Common causes of plantar fasciitis include biomechanical issues like flat feet or high arches, and overuse from activities such as running. Wearing shoes that lack proper support, tight calf muscles, and additional stress from excess body weight are other causes. Managing plantar fasciitis typically involves stretching exercises to relieve tension, wearing supportive footwear, and using orthotic inserts. Preventive measures focus on proper footwear and maintaining flexibility in the lower legs through regular stretching. If you are suffering from persistent heel pain, it’s suggested that you schedule an appointment with a podiatrist for an exam and suggestions for treatment, which can begin your journey to recovery and improved foot health.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
Safeguarding Diabetic Limbs
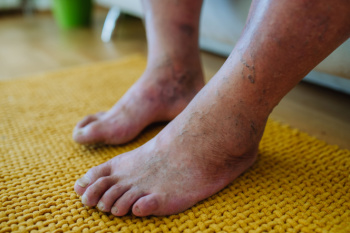
Preventing amputation of diabetic limbs is essential in preserving mobility and enhancing the quality of life for individuals with diabetes. Regular foot care plays a pivotal role in this endeavor. Daily inspection of the feet for cuts, blisters, or ulcers, along with proper hygiene and moisturization, helps detect issues early and prevent complications. Choosing appropriate footwear that fits well and provides adequate support reduces the risk of pressure points and injuries. Managing blood sugar levels through diet, exercise, and medication adherence is critical in preventing nerve damage and promoting wound healing. Seeking prompt medical attention for any foot problems, no matter how minor, is essential to prevent them from escalating into more serious issues. Regular check-ups with podiatrists allow for comprehensive monitoring of foot health and early intervention if problems arise. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can discuss important measures for limb protection.
Diabetic Limb Salvage
Diabetic limb salvage can be an effective way in preventing the need for limb amputation. If you have a foot ulcer and diabetes, consult with one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Diabetic Limb Salvage?
Diabetic limb salvage is the attempt of saving a limb, such as the foot, that has an infected ulcer, from amputation. Podiatrists also try to make sure that there is enough function in the foot after the salvage that it is still usable. Those with diabetes experience poor blood circulation, which prevents proper healing of an ulcer. If the ulcer is left uncheck, it could become infected, which could result in the need for amputation.
Diabetes is the number one cause of non-traumatic amputations in the United States. Amputation has been found to lead to higher mortality rates. This translates into higher healthcare costs, and a reduced quality of life and mobility for amputees. Podiatrists have attempted to increase the prevalence of limb salvage in an attempt to solve these issues.
Diagnosis and Treatment
Limb salvage teams have grown in recent years that utilize a number of different treatments to save the infected limb. This includes podiatrists that specialize in wound care, rehabilitation, orthotics, and surgery. Through a combination of these methods, limb salvage has been found to be an effective treatment for infected limbs, and as an alternative to amputation. Podiatrists will first evaluate the potential for limb salvage and determine if the limb can be saved or must be amputated.
If you have any questions, please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Diabetic Limb Salvage
Limb salvage is a procedure that involves saving a lower extremity from amputation. In podiatry, limb amputation often occurs as a result of diabetes. The fundamental goal of limb salvage is to restore and maintain stability and movement of the affected lower extremity.
The procedure typically involves removing the diseased tissue and a small portion of the surrounding healthy tissue, as well as the removal of any affected bone if necessary. If bone is removed it is then replaced with prostheses, or synthetic metal rods or plates, or grafts from either the patient’s body or a donor. Limb salvage is typically the preferred choice of procedure over amputation, as the procedure preserves both the patient’s appearance and allows for the greatest possible degree of function in the affected limb.
Upon diagnosis and determining that limb salvage is the appropriate treatment, the podiatrist may enlist the help of a physical and/or occupational therapist to prepare the patient for surgery by introducing various muscle-strengthening, walking, and range of motion exercises. Such exercises may be continued as rehabilitation post-procedure.
Dealing With Achilles Tendon Ruptures

Diagnosing Achilles tendon ruptures involves a combination of clinical evaluation and imaging tests. The Achilles tendon, the largest tendon in the body, connects the calf muscles to the heel bone. A rupture occurs when this tendon tears, often due to sudden or forceful movements during sports or activities that place excessive stress on the tendon. Symptoms of an Achilles tendon rupture typically include a sudden, sharp pain in the back of the ankle or calf, accompanied by swelling and difficulty walking or standing on tiptoe. While this injury can happen to anyone, factors such as age, sports participation, and pre-existing foot problems like flat feet or tendonitis may increase the risk. Treatment options include conservative measures like immobilization to more advanced options, like surgical repair for severe cases. If you have injured your Achilles tendon, it is strongly suggested that you schedule an appointment with a podiatrist for an accurate diagnosis and treatment plan.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact one of our podiatrists of Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
The Causes, Types, and Treatments of Achilles Tendon Injuries
Tendons are fibrous tissues that connect muscles with bone. The Achilles tendon is the largest tendon in the body. It connects the calf muscles at the back of the leg with the heel, and facilitates movements such as jumping, running, and walking.
Because the Achilles tendon is engaged so frequently and bears a great deal of pressure and stress throughout the day, it can become injured. Achilles tendon injuries cause the tissue to become irritated, inflamed, and swollen. Pain can come on gradually or be immediate, and will vary from mild to severe depending upon the injury. Where the pain occurs will vary as well, from just above the heel up through the back of the leg. There may also be stiffness in the tendon.
Achilles tendon injuries can often be caused by repetitive stress. They may also occur while running, playing tennis, gymnastics, football, basketball, dancing, soccer, baseball or other sports that require speeding up, slowing down, or pivoting quickly. Wearing high heels, falling from an elevation, stepping in a hole, having flat feet, bone spurs, tight leg muscles or tendons, wearing improper athletic shoes, exercising on uneven surfaces, or starting a new type of exercise can also cause Achilles tendon injuries.
The two most common Achilles tendon injuries are tendonitis and ruptures. Tendonitis causes painful inflammation and can occur in different parts of the tendon. Non-insertional Achilles tendonitis occurs when the fibers in middle of the tendon begin to break down, thicken, and swell. This condition typically affects younger, more active adults. Insertional Achilles tendonitis occurs where the tendon inserts into the heel bone. It is common for bone spurs to form with this type of injury. This condition can affect people of any age and level of activity.
Achilles tendon ruptures are a tear in the tendon. These breaks may be partial or complete. There may be an audible popping noise at the moment of injury and the pain will be sudden and severe.
An Achilles tendon injury can be diagnosed by your podiatrist after they examine you, check your range of motion, and possibly perform a calf squeeze test or review an X-ray or MRI. Depending on the type and severity of your injury, your podiatrist may treat your condition with rest/ice/compression/elevation (RICE), nonsteroidal anti-inflammatory medications, heel lifts, and stretching and strengthening exercises. If you have torn your Achilles tendon, treatment may include physical therapy, ultrasound, shockwave therapy, or possibly even surgery.
How Serious Is a Stubbed Toe?

A stubbed toe might seem like a minor inconvenience, but the pain it inflicts can be surprisingly intense. Stubbing your toe ranges from simple bruises to fractures, each with its own level of severity and potential complications. When you stub your toe, you are essentially subjecting it to sudden trauma. Common scenarios include accidentally ramming your toe into furniture or catching it on objects. Despite its seemingly innocuous nature, the impact can lead to a variety of injuries. Determining the extent of a stubbed toe injury is not always straightforward. Symptoms like intense pain, swelling, and difficulty while walking can accompany anything from a minor bruise to a fracture. The lack of immediate clarity underscores the importance of seeking professional help, particularly from a podiatrist. Bone bruises, strains, sprains, and toenail injuries are common consequences of stubbing a toe, each requiring different forms of treatment and management. Severe pain, swelling, visible deformities, or signs of infection warrant immediate attention. If you are suffering from toe pain, it is suggested that you make an immediate appointment with a podiatrist.
Toe pain can disrupt your daily activities. If you have any concerns, contact one of our podiatrists of Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Toe Pain
Toe pain can originate from corns, calluses, hammertoes, and bunions, as well as ingrown toenails, sprains, fractures, and dislocations. Corns develop as the toe rubs against the inside of a shoe which causes the skin to thicken as a form of protection. A corn is typically cone-shaped and has a small, hardened spot that points inward. When a corn is pressed into the skin, the toe becomes painful. Corns usually form on the top or side of the toe. A callus is also a thickened patch of skin that generally forms on the bottom of the foot. Calluses are the result of friction from the toe rubbing against the inside of a shoe. They may also occur by walking barefoot or having flat feet. A hammertoe is a bump on the knuckle of the second toe that is produced by wearing shoes that are too short for your feet. The bony protrusion rubs against the top of the shoe causing pain and irritation. A bunion is a malformation of the big toe. The base of the big toe pushes away from the smaller toes, forcing the top of the big toe to press toward the other toes. Bunions can be hereditary, or they can result from injury to the toe joint or from wearing high heels with a narrow toe box. The toe becomes inflamed, and a bump may develop at the end of the misplaced bone. Ingrown toenails typically affect the big toe and its surrounding skin. The nail will dig into the skin and become painful. Wearing tight or narrow shoes that compress the big toe causes the nail to grow into the fleshy part of the toe. Cutting toenails incorrectly can also add to the development of an ingrown toenail. A toe sprain originates from a torn or stretched ligament. Strapping the injured toe to the toe next to it for stabilization is common. A broken or fractured toe usually occurs from trauma like dropping a heavy object on it or bumping into something extremely hard and rigid. Osteoporosis, a thinning of the bones, can also bring about toe fractures.
Any of the conditions mentioned can lead to pain and irritation. While some are more serious than others, seeking an examination and diagnosis from a podiatrist is a good idea. A podiatrist can treat each ailment and get you back on your feet again without pain.
Ingrown Toenails in Children
 Ingrown toenails occur when the nail grows into the skin instead of over it, often the result of improper nail trimming, tight footwear, or injury. Ingrown toenails are common in children, as well as adults. The condition can cause pain, redness, and swelling around the child’s toe. If not treated properly, it can lead to infection. Especially for children, treatment typically begins conservatively, using methods such as soaking the affected foot in warm, soapy water to soften the nail and relieve pain. A podiatrist, or foot doctor, may try lifting the edge of the ingrown nail and placing a small amount of cotton underneath it to help guide the nail to grow above the skin. I is important for children to wear properly fitting shoes and to have their toenails trimmed straight across instead of rounded. This can help prevent the recurrence of ingrown toenails. If conservative treatments fail or if the ingrown toenail recurs frequently, a podiatrist may perform a minor procedure to remove part of the nail. They may treat the nail bed to prevent further issues, if necessary. This approach helps alleviate discomfort and prevent potential complications. If your child is suffering with an ingrown toenail, it is suggested you schedule an appointment with a podiatrist for prompt treatment.
Ingrown toenails occur when the nail grows into the skin instead of over it, often the result of improper nail trimming, tight footwear, or injury. Ingrown toenails are common in children, as well as adults. The condition can cause pain, redness, and swelling around the child’s toe. If not treated properly, it can lead to infection. Especially for children, treatment typically begins conservatively, using methods such as soaking the affected foot in warm, soapy water to soften the nail and relieve pain. A podiatrist, or foot doctor, may try lifting the edge of the ingrown nail and placing a small amount of cotton underneath it to help guide the nail to grow above the skin. I is important for children to wear properly fitting shoes and to have their toenails trimmed straight across instead of rounded. This can help prevent the recurrence of ingrown toenails. If conservative treatments fail or if the ingrown toenail recurs frequently, a podiatrist may perform a minor procedure to remove part of the nail. They may treat the nail bed to prevent further issues, if necessary. This approach helps alleviate discomfort and prevent potential complications. If your child is suffering with an ingrown toenail, it is suggested you schedule an appointment with a podiatrist for prompt treatment.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact one of our podiatrists of Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.