Featured Articles

How Is Plantar Fasciitis Diagnosed?
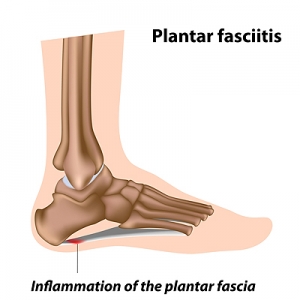
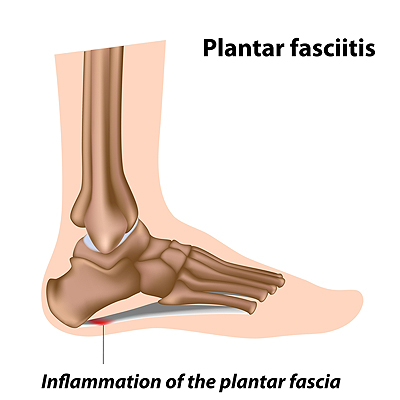 Plantar fasciitis is a common cause of foot pain. It is caused by an inflammation of the plantar fascia, a ligament that runs along the bottom of the foot, connecting the heel to the toes. Getting a diagnosis of plantar fasciitis begins with a trip to the podiatrist. The doctor will typically conduct a patient interview and ask you to talk about your medical history, your current symptoms, and how your foot pain is affecting your daily activities. The doctor will then complete a physical examination of your foot, taking note of issues like swelling, tenderness, pain points, and range of motion. The doctor may also ask you to walk around the room to examine your gait. Imaging studies, such as X-rays or MRIs, can help confirm a diagnosis of plantar fasciitis and rule out other conditions, such as a heel fracture. If you are experiencing foot pain, it is recommended that you seek the care of a podiatrist.
Plantar fasciitis is a common cause of foot pain. It is caused by an inflammation of the plantar fascia, a ligament that runs along the bottom of the foot, connecting the heel to the toes. Getting a diagnosis of plantar fasciitis begins with a trip to the podiatrist. The doctor will typically conduct a patient interview and ask you to talk about your medical history, your current symptoms, and how your foot pain is affecting your daily activities. The doctor will then complete a physical examination of your foot, taking note of issues like swelling, tenderness, pain points, and range of motion. The doctor may also ask you to walk around the room to examine your gait. Imaging studies, such as X-rays or MRIs, can help confirm a diagnosis of plantar fasciitis and rule out other conditions, such as a heel fracture. If you are experiencing foot pain, it is recommended that you seek the care of a podiatrist.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
How to Prevent Athlete's Foot
 Athlete’s foot is a fungal infection of the skin on the feet. It can cause redness, flakiness, peeling, or cracking of the skin on the feet and may also itch, sting, or burn. Fortunately, this type of infection can be prevented. Fungus thrives in moist environments, so always thoroughly dry your feet after getting them wet, especially between the toes. Choose well-ventilated or moisture-wicking shoes and socks to help keep your feet dry. You can also use a powder on the feet everyday to keep them dry. People often catch the fungus that causes athlete’s foot from walking barefoot through wet areas, so when walking through a public area like a locker room or pool, wear water-proof shoes or flip-flops. If you suspect that you have athlete’s foot, it is suggested that you see a podiatrist for treatment.
Athlete’s foot is a fungal infection of the skin on the feet. It can cause redness, flakiness, peeling, or cracking of the skin on the feet and may also itch, sting, or burn. Fortunately, this type of infection can be prevented. Fungus thrives in moist environments, so always thoroughly dry your feet after getting them wet, especially between the toes. Choose well-ventilated or moisture-wicking shoes and socks to help keep your feet dry. You can also use a powder on the feet everyday to keep them dry. People often catch the fungus that causes athlete’s foot from walking barefoot through wet areas, so when walking through a public area like a locker room or pool, wear water-proof shoes or flip-flops. If you suspect that you have athlete’s foot, it is suggested that you see a podiatrist for treatment.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Athlete’s Foot
Athlete’s foot, or tinea pedis, is a skin disease caused by a fungal infection. The infection typically occurs between the toes, and the feet are most subject to this disease because shoes best create the warm, dark, and moist environment in which fungus thrives. Other areas that create a similar environment, such as swimming pools, public showers, and locker rooms; can also promote fungi growth.
Symptoms of athlete’s foot include dry skin, itching, scaling, inflammation, and blistering. Sometimes, blisters can evolve into the cracks or breaks in the skin. The exposed tissue can then create pain, swelling, and discharge. The spread of infection can cause itching and burning as well.
While athlete’s foot commonly occurs between the toes, it may also spread to the toenails or soles of the feet. Other parts of the body, such as the groin or underarms, can also become infected if they are touched after the original area of infection is scratched. Aside from physical contact, athlete’s foot can also spread through the contamination of footwear, clothing or bedsheets.
Proper foot hygiene is essential in preventing athlete’s foot. You can prevent the fungus from spreading by frequently washing your feet using soap and water, thoroughly drying the feet between the toes, changing shoes and socks every day to reduce moisture, and ensuring that bathroom and shower floors are disinfected. Other tips include using shower shoes, avoiding walking barefoot in public environments, wearing light and airy shoes, and wearing socks that keep the feet dry.
While treatment for athlete’s foot can involve topical or oral antifungal drugs, mild cases of the infection can be treated by dusting foot powder in shoes and socks. Any treatment used can be supplemented by frequently bathing the feet and drying the toes. If proper foot hygiene and self-care do not ease your case of athlete’s foot, contact your podiatrist. He will determine if the underlying cause of your condition is truly a fungus. If that is the case, a comprehensive treatment plan may be suggested with the inclusion of prescription antifungal medications.
Staying a Step Ahead of Diabetic Foot Problems
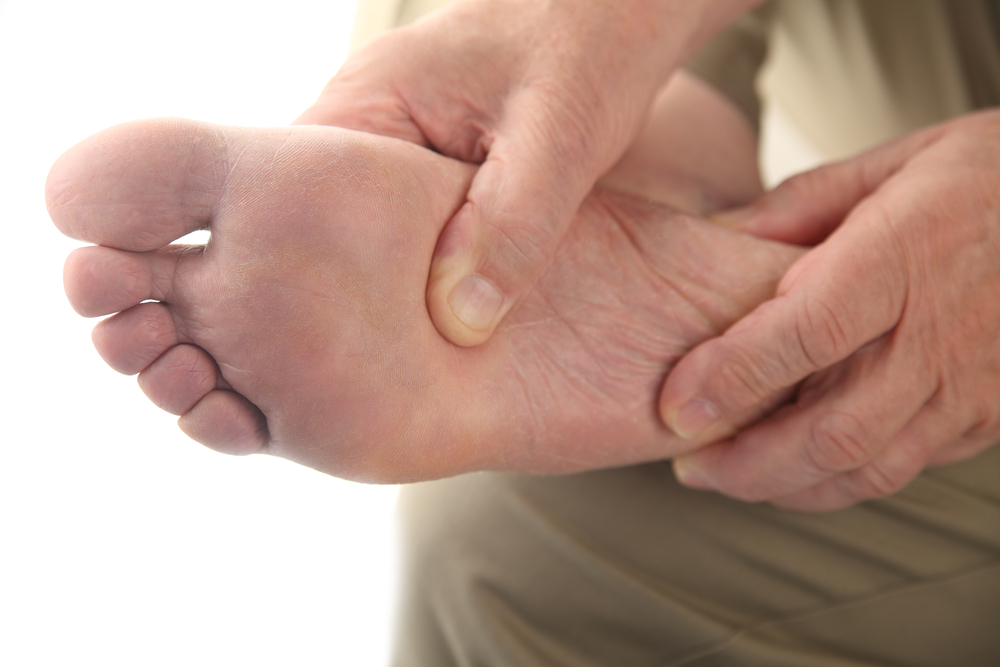 Though it is a metabolic disorder, diabetes can have serious implications for your foot health. Diabetes can cause the feet to be less sensitive and slow to heal from damage, which can result in complications such as diabetic foot ulcers. Fortunately, there are precautions that you can take to get ahead of many diabetic foot problems. If you have diabetes, it is recommended that you perform daily foot checks to see if you have any cuts, sores, or blisters so that you can treat them immediately and avoid infections. Keep your feet clean by washing them daily and drying them thoroughly, then apply a thin layer of lotion to the tops and bottoms of the feet, avoiding the areas between your toes where the extra moisture can help fungus thrive. Regularly trim your toenails straight across to avoid ingrown nails, and wear comfortable shoes instead of going barefoot. If you have a history of diabetes-related foot problems, it is suggested that you are under the care of a podiatrist who can help you take care of your feet.
Though it is a metabolic disorder, diabetes can have serious implications for your foot health. Diabetes can cause the feet to be less sensitive and slow to heal from damage, which can result in complications such as diabetic foot ulcers. Fortunately, there are precautions that you can take to get ahead of many diabetic foot problems. If you have diabetes, it is recommended that you perform daily foot checks to see if you have any cuts, sores, or blisters so that you can treat them immediately and avoid infections. Keep your feet clean by washing them daily and drying them thoroughly, then apply a thin layer of lotion to the tops and bottoms of the feet, avoiding the areas between your toes where the extra moisture can help fungus thrive. Regularly trim your toenails straight across to avoid ingrown nails, and wear comfortable shoes instead of going barefoot. If you have a history of diabetes-related foot problems, it is suggested that you are under the care of a podiatrist who can help you take care of your feet.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Conditions
According to the American Diabetes Association (ADA), diabetes is a condition that affects approximately 23.6 million Americans. Around 750,000 new cases are diagnosed each year, and the disease’s most common form, Type 2 diabetes, makes up for 90 to 95 percent of these cases. Type 2 diabetes is especially prevalent among older Americans, those who are obese, and those who lead sedentary lifestyles.
Complications of the disease may lead to several foot and ankle-related conditions. The loss of nerve sensation, or neuropathy, can cause diabetics to lose feeling at the bottom of the feet and therefore leave them unaware of pain, pressure, and heat. Decreased circulation is another complication of diabetes that can slow down the healing of wounds and injuries; this can lead to the development of foot ulcers.
To prevent foot ulcers from forming, diabetics should examine their feet every day for small cuts and wear shoes that curtail pressure. Constant monitoring for the risk factors associated with ulcer formation can allow for early detection and therefore lessen the possibility of ulcers or, even worse, amputation. The removal of calluses and ingrown toenails should be left to the podiatrist to avoid improper removal and possible infection.
Diabetic patients may also experience foot deformities due to complications in their feet, such as limited joint mobility, muscle atrophy, and decreased fat padding. These complications can increase pressure in certain areas of the foot, which in turn can cause certain deformities, such as hammertoe, to form. Another deformity, Charcot foot, develops due to the collapsing of microfractures in the bones of the feet. The resulting deformity is a foot that is flattened and wider in appearance.
To help minimize pressure and prevent the development of these diabetes-related foot and ankle conditions, your podiatrist may consider using orthotics or special shoes. Charcot foot may be treated using walkers, custom orthotic insoles, or non-weight-bearing or rigid weight-bearing casts or braces. In more serious cases, surgery may be considered to treat more developed deformities. Ulcers can be further cared for with the help of proper diet, medication to control glucose, intensive wound care, and infection treatment.
How to Get a Proper Shoe Fit
Many people suffer from foot problems because their shoes are poorly fitted. When shopping for a new pair of shoes, fashion usually triumphs over comfortability. A pair of well fitted shoes is essential in preventing foot problems and potential injuries.
Poorly fitted shoes can cause foot issues such as plantar fasciitis, bunions, hammertoes, ingrown toenails, and foot pain. Shoes such as high heels and sandals may cause problems for your feet. These shoes put the foot in an unnatural position for long periods and fail to provide good foot support. It is recommended to not wear either one for an extended period.
When you are trying on shoes, make sure they have enough space for your toes to move around. Shoes shouldn’t be cramped but also shouldn’t have too much room that your foot moves around in them. A snug shoe is a good choice. They should also provide good arch support and cushioning. Athletic shoes tend to offer both good support and cushioning. A degree of flexibility is necessary so they aren’t too stiff or too unsupportive.
If you can wear your shoes for a long period of time without experiencing any discomfort, this is a sign that your shoes fit properly. Do not be too dismayed if the shoe isn’t a perfect fit at first; many shoes take a few days to weeks to properly break in. However don’t expect an uncomfortable shoe to become fitted to your foot.
For those with foot conditions such as flat feet or pronation, orthotics may be helpful or even necessary to prevent foot pain. Orthotics are inserts that are placed in the shoe and provide support and cushioning for the foot. While there are many types of orthotics out there, custom-made orthotics may be necessary depending upon your foot and foot conditions.
Feet change in size over time. It is important to check your foot size over time so that you can make sure you have the perfect fit for your feet. A podiatrist can provide more information on proper shoe fitting and foot orthotics.
All About Bunions
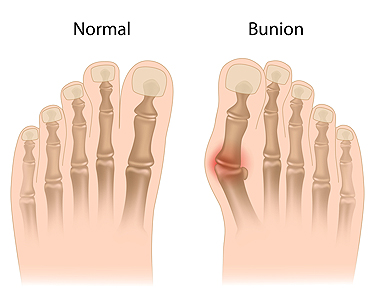 Bunions are a deformity of the toe joint that cause the big toe to move towards the other toes. The most common complaints of people with bunions are pain, a prominent bulge on the side of their foot, and difficulty wearing shoes. Bunions tend to get progressively worse over time, so it is important to seek medical care. A podiatrist diagnoses bunions by examining the foot, and may then take an X-ray to determine the severity of the condition. The doctor may recommend conservative care to manage the symptoms, or surgery to correct the deformity. If you suspect you have a bunion, it is recommended that you speak with a podiatrist who can diagnose and treat your condition.
Bunions are a deformity of the toe joint that cause the big toe to move towards the other toes. The most common complaints of people with bunions are pain, a prominent bulge on the side of their foot, and difficulty wearing shoes. Bunions tend to get progressively worse over time, so it is important to seek medical care. A podiatrist diagnoses bunions by examining the foot, and may then take an X-ray to determine the severity of the condition. The doctor may recommend conservative care to manage the symptoms, or surgery to correct the deformity. If you suspect you have a bunion, it is recommended that you speak with a podiatrist who can diagnose and treat your condition.
If you are suffering from bunions, contact one of our podiatrists of Romeo Foot & Ankle Clinic. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
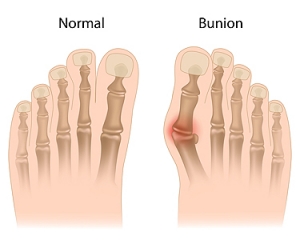
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
Stretching to Reduce Heel Pain
 Plantar fasciitis, a condition in which the plantar fascia ligament that runs along the bottom of your foot becomes inflamed, is one of the most common causes of heel pain among adults. Fortunately, something as simple as stretching your feet can help prevent plantar fasciitis, all while increasing the strength and flexibility of your feet. One easy stretch that you can do in the comfort of your own home is the Water Bottle Stretch. To do this stretch, sit down in a chair and place a water bottle, tennis ball, or rolling pin on the floor in front of you. Slowly roll the bottom of your foot over the object, starting from the ball of your foot and moving back towards the heel. Do this for about a minute, and then repeat on the other foot. If you are using a water bottle, you may also freeze it prior to doing this stretch. The cold water bottle will then simultaneously stretch and ice your foot, reducing pain and inflammation. For more information on how you can prevent plantar fascia injuries and for treatment options for plantar fasciitis, consult with a podiatrist today.
Plantar fasciitis, a condition in which the plantar fascia ligament that runs along the bottom of your foot becomes inflamed, is one of the most common causes of heel pain among adults. Fortunately, something as simple as stretching your feet can help prevent plantar fasciitis, all while increasing the strength and flexibility of your feet. One easy stretch that you can do in the comfort of your own home is the Water Bottle Stretch. To do this stretch, sit down in a chair and place a water bottle, tennis ball, or rolling pin on the floor in front of you. Slowly roll the bottom of your foot over the object, starting from the ball of your foot and moving back towards the heel. Do this for about a minute, and then repeat on the other foot. If you are using a water bottle, you may also freeze it prior to doing this stretch. The cold water bottle will then simultaneously stretch and ice your foot, reducing pain and inflammation. For more information on how you can prevent plantar fascia injuries and for treatment options for plantar fasciitis, consult with a podiatrist today.
Why Stretching Is Important for Your Feet
Stretching the feet is a great way to prevent injuries. If you have any concerns with your feet consult with one of our podiatrists from Romeo Foot & Ankle Clinic. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Stretching the Feet
Stretching the muscles in the foot is an important part in any physical activity. Feet that are tight can lead to less flexibility and make you more prone to injury. One of the most common forms of foot pain, plantar fasciitis, can be stretched out to help ease the pain. Stretching can not only ease pain from plantar fasciitis but also prevent it as well. However, it is important to see a podiatrist first to determine if stretching is right for you. Podiatrists can also recommend other ways to stretch your feet. Once you know whether stretching is right for you, here are some excellent stretches you can do.
- Using a foam roller or any cylindrical object (a water bottle or soda can will do), roll the object under your foot back and forth. You should also exert pressure on the object. Be sure to do this to both feet for a minute. Do this exercise three times each.
- Similar to the previous exercise, take a ball, such as a tennis ball, and roll it under your foot while seated and exert pressure on it.
- Grab a resistance band or towel and take a seat. If you are using a towel, fold it length wise. Next put either one between the ball of your foot and heel and pull with both hands on each side towards you. Hold this for 15 seconds and then switch feet. Do this three times for each foot.
- Finally hold your big toe while crossing one leg over the other. Pull the toe towards you and hold for 15 seconds. Once again do this three times per foot.
It is best to go easy when first stretching your foot and work your way up. If your foot starts hurting, stop exercising to ice and rest the foot. It is advised that you then see a podiatrist for help.
If you have any questions, please feel free to contact our offices located in Washington and Shelby Townships, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.